Why the words we use matter, and why one dog’s story changed how I talk about vaccines
By Dr. Elena Shockman

If you’ve spent any time in pet wellness spaces lately, whether online, in a pet store, or chatting with a neighbor at the dog park, you’ve probably heard “integrative” and “holistic” used interchangeably. Both words sound reassuring. They aren’t the same thing, though, and mixing them up can have real consequences. I watched those consequences play out during one of the most heartbreaking nights of my veterinary training.
I’m not here to lecture anyone. I understand the impulse to question standard medicine, to want “natural” options, to be skeptical of vaccines and pharmaceuticals in a world saturated with misinformation in both directions. But I do want to draw a clear, science-grounded line between approaches that can meaningfully complement conventional veterinary care, and a philosophy that, taken to an extreme, can put animals at serious risk.
So, the terminology…
What “integrative” actually means
Integrative veterinary medicine is evidence-informed. It takes the best of conventional Western medicine (diagnostics, pharmaceuticals, surgery) and combines it thoughtfully with alternative modalities that have a meaningful body of scientific or observational data behind them. The word integrative is doing real work here. These approaches are added to conventional care, not substituted for it.
Some examples of alternative modalities with legitimate scientific support:

- Veterinary acupuncture: Recognized by the AVMA and supported by a growing body of peer-reviewed research, acupuncture has demonstrated efficacy in managing chronic pain, neurological conditions, and certain musculoskeletal disorders. It’s used frequently in rehabilitation medicine and for palliative care in cancer patients.
- Rehabilitation therapy (veterinary physical therapy): Post-surgical recovery, degenerative joint disease, and neurological rehab have all benefited from structured physiotherapy protocols. This is evidence-based medicine that happens to use non-pharmaceutical tools.
- Laser (photobiomodulation) therapy: Increasingly well-studied for wound healing, pain reduction, and inflammation management. Widely used in conjunction with conventional treatment, especially for orthopedic conditions.
- Veterinary chiropractic and spinal manipulation: Has observational data supporting use in select musculoskeletal and neurological cases when performed by a credentialed practitioner (AVCA-certified).
- Evidence-supported nutraceuticals: Omega-3 fatty acids, glucosamine/chondroitin in appropriate formulations, and certain probiotics have peer-reviewed data behind them for specific conditions. They aren’t magic bullets, but they aren’t snake oil either.
- Veterinary massage and hydrotherapy: Particularly useful in rehabilitation contexts, with observational and emerging clinical evidence for their role in recovery and chronic pain management.
The common thread? These modalities are used alongside conventional medicine, and they’re evaluated using the same scientific rigor we’d apply to any treatment. The question isn’t “is this natural?” The question is “does the evidence support this for this patient?”
What “holistic” often means in practice

The word “holistic” literally means considering the whole: the whole patient, the whole environment, the whole lifestyle. That principle is something I fully agree with. Modern veterinary medicine absolutely should be looking at the whole animal, not just the presenting symptom.
In practice, though, “holistic veterinary medicine” has often become less a scientific framework and more a philosophy. Sometimes a lifestyle identity. And it can drift into anti-vaccine territory, rejection of conventional diagnostics, and promotion of unproven treatments simply because they’re “natural.”
Here I have to be direct: natural does not equal safe, and conventional does not equal harmful. Arsenic is natural. Parvo is natural. Homeopathy, which operates on principles that contradict basic chemistry and physics, is not supported by credible clinical evidence despite decades of study.
When “holistic” becomes a lens through which all conventional medicine is viewed with suspicion, and all “natural” alternatives are accepted uncritically, it stops being a philosophy of whole-patient wellness. It becomes something that can genuinely harm animals.
I know that because I’ve seen it happen.
The night ten dogs got parvo
It was a Friday night during my emergency rotation at Penn Vet. The phone rang. On the other end was a frantic woman, a Shar-Pei breeder who had taken her dogs to a holistic veterinarian. On that vet’s recommendation, none of her ten dogs had been vaccinated. She wasn’t negligent or careless. She trusted her vet. She believed she was doing what was best for her animals.
She also worked at a pet rescue.
There had been a parvovirus case at the rescue that week. Parvo is one of the most environmentally stable and contagious pathogens in veterinary medicine. It can survive on surfaces, clothing, and shoes for months to years. Without realizing it, she had carried it home.
All ten of her dogs were violently ill. Profuse vomiting. Hemorrhagic diarrhea. One dog was in critical condition, deteriorating rapidly on the drive to the ER.

We were scrambling. Parvovirus requires strict isolation. It is extraordinarily contagious and can devastate an entire hospital population if containment fails. Our isolation unit had a maximum capacity of three animals. We had ten coming in.
One dog didn’t make it. He died on the way to us.
The remaining nine were hospitalized across multiple facilities and treated with aggressive supportive care: IV fluids, gastroprotectants, antiemetics, nutritional support, around-the-clock monitoring. There is no antiviral treatment for parvo. You’re essentially keeping the animal alive long enough for their immune system to mount a response. It’s labor-intensive, and it’s expensive.
The nine surviving dogs all made it. But I would not be surprised if that owner is still paying off her credit card bill fifteen years later.
The worst part, and I mean this sincerely, is that every single bit of this was preventable.
The DHPP vaccine (distemper, hepatitis, parvovirus, parainfluenza) is one of the most rigorously studied vaccines in veterinary medicine. It works. It has decades of safety data behind it. It’s a core vaccine for dogs precisely because the diseases it prevents are severe, widespread, and, in the case of parvo, brutally difficult to treat.
I’m not a vaccine zealot, but let’s talk about core vs. lifestyle vaccines
I want to be clear about something: I am not someone who believes every pet needs every vaccine on a rigid, one-size-fits-all schedule. That kind of blanket thinking is not actually how good veterinary medicine works. One of the most important distinctions we make in practice is between core vaccines and lifestyle vaccines. This is one place where veterinary medicine is actually more nuanced than human medicine.
Core vaccines
Core vaccines are recommended for virtually all dogs and cats regardless of lifestyle, because the diseases they prevent are severe, highly contagious, or carry significant public health implications. For dogs, these include:
- DHPP (distemper, hepatitis, parvovirus, parainfluenza)
- Rabies (also required by law in most jurisdictions, because rabies is fatal and transmissible to humans)
For cats, core vaccines include FVRCP (feline viral rhinotracheitis, calicivirus, panleukopenia) and rabies. These are the vaccines that, in my opinion and in the opinion of the AAHA and AVMA, should not be skipped without an extraordinary medical reason (such as a documented prior adverse reaction or a documented terminal illness).
Lifestyle vaccines
Lifestyle vaccines, on the other hand, are recommended based on a pet’s individual risk profile. This is where the conversation gets genuinely individualized, and where I actually enjoy talking with pet owners about their animal’s life.
For example:
- Bordetella (kennel cough): Recommended for dogs who attend daycare, board regularly, go to dog parks, or are frequently exposed to other dogs. Not necessarily required for a dog who lives in a rural setting with minimal social contact.
- Leptospirosis: Recommended for dogs who hike, swim in natural water sources, or live in areas with known wildlife exposure. Less relevant for an urban apartment dog.
- Lyme disease: Strongly recommended in tick-endemic regions, especially for outdoor dogs.
- Canine influenza (H3N8 / H3N2): Recommended during known outbreaks or for dogs with high social exposure in areas where the virus is circulating.
This risk-based approach is fundamentally different from how vaccines work in human public health, where broader population-level immunity is the primary goal and schedules are more standardized. In veterinary medicine, we have the luxury, and the responsibility, of truly tailoring recommendations to each individual animal’s life. It’s something I genuinely love about the practice.
Where I actually stand
I believe in the art and science of whole-patient medicine. A dog’s diet, environment, stress level, genetics, and social life matter enormously to their health outcomes. Some alternative modalities (acupuncture, rehabilitation therapy, targeted nutraceuticals) have genuine value and deserve a place in modern veterinary care.
I also believe that a well-designed, individualized vaccine protocol is one of the most consequential things you can do for your pet. Not because I’m reflexively pro-pharmaceutical. Because I have seen, with my own eyes, what happens when highly effective vaccines are withheld on the basis of philosophy rather than evidence.
I think about those ten Shar-Peis often. I think about the dog who didn’t make it. I think about a caring owner who trusted her veterinarian and was failed by a philosophy that prioritized “natural” over “evidenced.”
The integrative approach I practice and advocate for doesn’t ask you to choose between “conventional” and “alternative.” It asks a better question: what does the evidence say, and what does this specific patient need?
That, to me, is what real whole-patient care looks like.
Have questions about your pet’s vaccine protocol or integrative care options? Reach out! I’m always happy to talk through what makes sense for your individual animal.
With love as always,
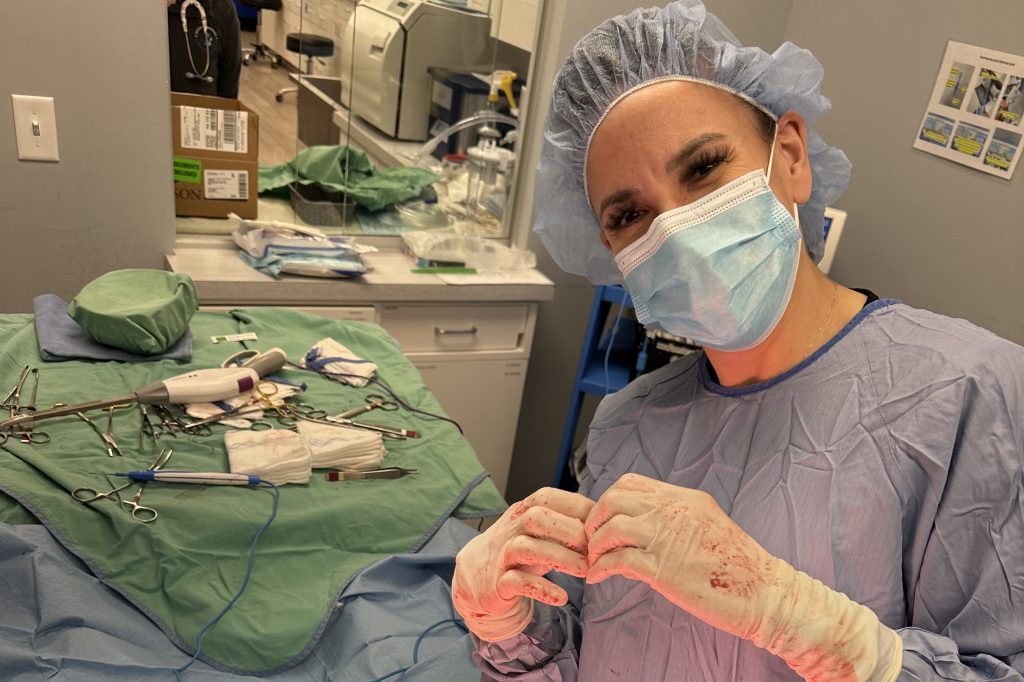
-Dr. Elena Shockman, VMD, Founder of Paw & Pestle




Leave a comment